The escalating prevalence of human papillomavirus (HPV) and its direct correlation with anogenital malignancies has necessitated a profound shift in preventive healthcare strategies. As the incidence of anal squamous cell carcinoma continues a concerning upward trajectory, the medical community has pivoted toward highly specialized, proactive diagnostic interventions. At the center of this clinical evolution is a procedure uniquely designed to intercept precancerous cellular transformations before they reach malignancy. This comprehensive clinical report examines the intricate mechanisms, epidemiological significance, patient indications, and procedural workflows surrounding High-Resolution Anoscopy (HRA).
Providing these critical services requires a sophisticated synthesis of infectious disease expertise, advanced optical technology, and culturally competent patient care. Farabi Wellness Center stands as a premier diagnostic facility addressing this urgent public health mandate. Under the medical direction of Dr. Alireza Farabi, the institution integrates evidence-based screening protocols with state-of-the-art colposcopic instrumentation to deliver unparalleled preventive care. This exhaustive guide serves to elucidate the profound medical importance of HRA, detailing its application for at-risk demographics and outlining the comprehensive care paradigms available within the local healthcare landscape.
What is HRA?
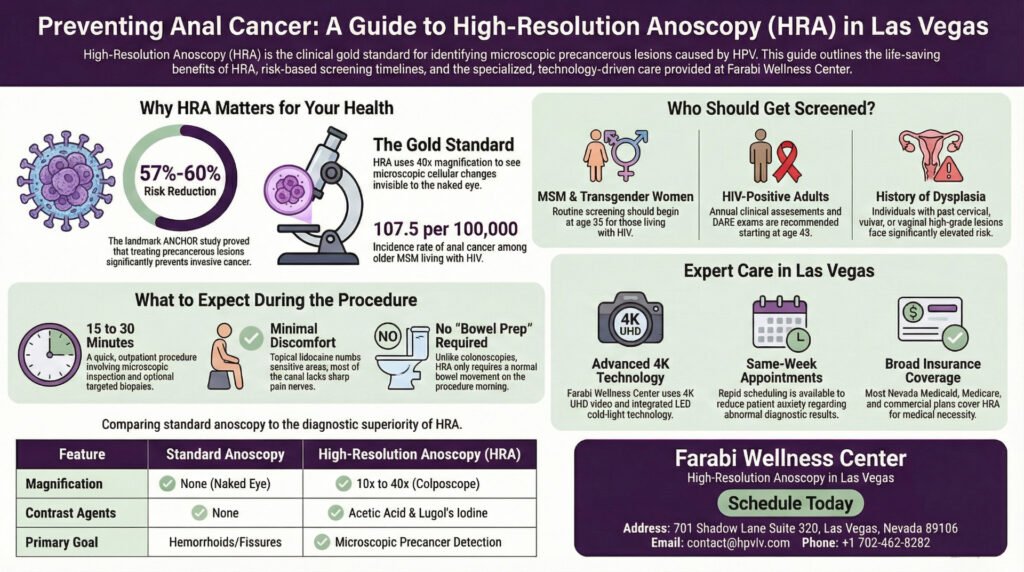
What is High-Resolution Anoscopy (HRA)? High-Resolution Anoscopy (HRA) is the clinical gold standard procedure utilized for the meticulous examination, identification, and targeted treatment of anal dysplasia, also known as anal intraepithelial neoplasia (AIN). Utilizing a specialized magnifying instrument known as a colposcope, alongside the application of precise chemical contrast agents like acetic acid and Lugol’s iodine, HRA allows clinicians to visualize microscopic precancerous cellular anomalies that are entirely invisible to the naked eye during standard examinations. By detecting these cellular changes early, healthcare providers can execute targeted biopsies and initiate ablative therapies, effectively preventing the progression of dysplasia into invasive anal squamous cell carcinoma.
To fully grasp the diagnostic superiority of HRA, it must be distinctly separated from other common gastrointestinal and colorectal examinations. Standard anoscopy relies on a simple, short, rigid tubular instrument to visually inspect the anal canal. While standard anoscopy is highly effective for identifying macroscopic pathologies such as hemorrhoids, structural fistulas, fissures, and large tumors, it completely lacks the optical magnification required to observe the cellular architecture of the mucosal lining. Similarly, colonoscopies—while universally implemented for colorectal cancer screening—utilize flexible endoscopes designed to traverse the entire colon to identify adenomatous polyps. Colonoscopes are structurally and optically ill-equipped to perform microscopic evaluations of the squamous epithelium situated in the immediate anal canal.
High-Resolution Anoscopy bridges this critical diagnostic void by adapting the proven principles of cervical colposcopy to the anorectal region. The procedure integrates a high-resolution colposcope, a stereoscopic binocular field microscope that provides intense, focused LED illumination and magnification capabilities ranging from 10x to over 40x. This extraordinary magnification allows the examining physician to meticulously scrutinize the vascular patterns and epithelial topography of the anal transformation zone. When combined with chemical biomarkers, the technology clearly delineates the margins between healthy, mature squamous cells and dysplastic tissue characterized by high nuclear density. This seamless integration of optics and biochemistry ensures that high-grade lesions are immediately identified, paving the way for.
Why HRA Matters in HPV Detection
The fundamental imperative for High-Resolution Anoscopy is intrinsically linked to the pathophysiology of the human papillomavirus. HPV is the most ubiquitous sexually transmitted infection globally, with epidemiological data indicating that at least fifty percent of sexually active individuals will contract a genital or anal HPV infection during their lifetime. While the human immune system successfully clears the vast majority of these transient infections within one to two years, a subset of patients experiences persistent, chronic infections with high-risk oncogenic strains, predominantly HPV-16 and HPV-18.
The anal canal features a distinct anatomical region known as the transformation zone, where the glandular columnar epithelium of the lower rectum abruptly transitions into the squamous epithelium of the anal verge. This transitional tissue is exceptionally vulnerable to viral integration. When high-risk HPV infiltrates the basal layer of this epithelium, the viral genome begins expressing the E6 and E7 oncoproteins. These malicious viral proteins systematically dismantle the host cell’s regulatory mechanisms by binding to and inactivating crucial tumor suppressor genes, specifically p53 and the retinoblastoma protein (pRb). The inactivation of these regulatory checkpoints leads to unregulated, rapid cellular proliferation and the accumulation of genetic mutations over time. This continuous cellular disruption clinically manifests as progressive anal dysplasia, escalating from Low-grade Squamous Intraepithelial Lesions (LSIL) to High-grade Squamous Intraepithelial Lesions (HSIL), and ultimately, if left entirely unchecked, to invasive anal squamous cell carcinoma.
Epidemiological Context and Regional Data
The transition from persistent HPV infection to invasive cancer is a slow, insidious process that typically spans decades. However, the aggregate impact of these infections has resulted in a demonstrable increase in anal cancer rates. Nationwide, the incidence of anal cancer has escalated steadily, with researchers noting an average annual increase of 1.7% to 2.7% over the last forty years.
Within the state of Nevada, data meticulously maintained by the Nevada Central Cancer Registry and the federal SEER database reflects this concerning national trend. While anal cancer remains a relatively rare malignancy compared to colorectal or lung cancers, its localized incidence demands specialized public health interventions. The necessity for a dedicated infrastructure is evident when analyzing the statistical burden placed upon urban centers like Clark County.
| Epidemiological Variable | Clark County (Urban) | Nevada Statewide | National Average (US SEER) |
| Incidence Rate (per 100,000) | 5.3 to 7.0 | 5.5 to 7.3 | 6.3 to 8.4 |
| Mortality Rate (per 100,000) | 1.1 | 1.3 | 1.8 |
| Trend Direction | Stable | Stable | Rising |
| Primary Etiological Factor | HPV Infection | HPV Infection | HPV Infection |
Data derived from the State Cancer Profiles and the Nevada Central Cancer Registry, capturing age-adjusted rates for regional and distant staging.
While the general incidence rate in Nevada hovers around 5.5 to 7.3 per 100,000 individuals, these aggregated figures obscure the profound vulnerability of specific, high-risk subpopulations whose incidence rates eclipse the general average by staggering margins.
The ANCHOR Study: A Clinical Paradigm Shift
The medical justification for implementing widespread HRA programs was unequivocally cemented by the landmark Anal Cancer/HSIL Outcomes Research (ANCHOR) trial, the results of which were published in the New England Journal of Medicine in 2022. Prior to the culmination of this extensive, multi-site clinical trial, the medical oncology community was deeply divided regarding the optimal management strategy for anal HSIL. While cervical dysplasia is routinely ablated to prevent cervical cancer, it was historically unclear whether treating anal dysplasia would yield a similar prophylactic benefit, or if a conservative strategy of “watchful waiting” was equally effective.
The ANCHOR study definitively resolved this clinical ambiguity. The trial was statistically powered to determine if the active identification and treatment of anal HSIL (utilizing HRA-guided therapies such as electrocautery or laser ablation) could reduce the incidence of invasive anal cancer by at least fifty percent. The results were resoundingly clear: treating precancerous anal lesions reduced the subsequent risk of developing invasive anal cancer by approximately 57% to 60% when compared directly to the active monitoring cohort.
This revelation constituted a monumental paradigm shift in infectious disease and oncology protocols. The evidence generated by the ANCHOR trial conclusively proved that anal cancer is highly preventable, provided that clinicians actively hunt for and eradicate the precursor lesions. Consequently, HRA is no longer viewed as an optional, exploratory diagnostic tool; it is now universally recognized as an indispensable, life-saving intervention that must be integrated into the standard of care for all high-risk patients.
Who Needs HRA?
Identifying the specific patient populations that require High-Resolution Anoscopy is a critical exercise in evidence-based risk stratification. Because the baseline incidence of anal squamous cell carcinoma in the general, uninfected public is exceedingly low—averaging approximately 1.5 to 1.7 cases per 100,000 person-years—universal, population-wide HRA screening is neither clinically indicated nor economically feasible. Instead, public health authorities rely on highly targeted screening algorithms designed to intercept the disease in demographics where the statistical prevalence of HPV and resultant HSIL is magnified.
In early 2024, the International Anal Neoplasia Society (IANS), operating in close collaboration with federal entities including the CDC, the NIH Office of AIDS Research Advisory Council, and the Infectious Diseases Society of America (IDSA), published comprehensive, unified guidelines for anal cancer screening. These sweeping guidelines stratify patients into meticulous risk categories based on their statistical likelihood of developing the disease.
The guidelines emphasize that screening should commence with a thorough assessment of clinical symptoms, a Digital Anorectal Examination (DARE), and a laboratory-based anal cytology swab. This can be part of Routine Sexual Health Screenings for people at elevated risk. If the cytology reveals any degree of cellular abnormality, or if high-risk HPV DNA is detected via co-testing, the patient must be immediately referred to a specialized facility for an HRA.
Risk Category A: The Highest Priority Demographics
Risk Category A encompasses distinct patient populations whose incidence of anal cancer is at least ten times higher than that of the general United States population, crossing the threshold of 17 cases per 100,000 person-years. For these individuals, routine, proactive screening is an absolute medical necessity.
The primary demographics within Risk Category A include men who have sex with men (MSM) and transgender women living with HIV. The guidelines issue a stringent recommendation that these individuals must initiate routine screening no later than age 35, owing to a profoundly elevated incidence rate that consistently exceeds 70 cases per 100,000 person-years. Similarly, women and men who have sex with women who are living with HIV are instructed to commence screening protocols by age 45. Even in the absence of an HIV diagnosis, MSM and transgender women face an elevated risk due to behavioral and physiological factors and are advised to begin screening at age 45.
Beyond the parameters of sexual health and infectious disease, Risk Category A also explicitly includes individuals with a documented history of severe anogenital dysplasia. Women who have previously been diagnosed with vulvar, vaginal, or cervical high-grade squamous intraepithelial lesions (HSIL) or invasive cancers face an anal cancer incidence rate exceeding 40 per 100,000. This elevated risk is attributed to the “field effect” of HPV, wherein the viral pathogen creates widespread, multifocal reservoirs of dysplastic tissue across the contiguous epithelium of the entire lower genital and anogenital tract. Furthermore, individuals who have undergone solid organ transplantation and have survived ten years post-transplant are classified within this highest risk tier, driven by the profound, long-term pharmacological immunosuppression required to prevent organ rejection.
Risk Category B: Elevated Surveillance Demographics
Risk Category B identifies individuals who possess a statistically significant, elevated risk of anal neoplasia compared to the general public, though their incidence rates do not quite breach the ten-fold threshold required for Category A. For these patients, the implementation of screening protocols should be established through shared clinical decision-making between the patient and their provider.
This secondary category encompasses individuals aged 45 and older who exhibit a history of persistent, unresolved cervical HPV-16 infections. It also includes patients who have suffered from recurrent perianal warts (condyloma acuminata), as the presence of benign warts strongly indicates a prior inability to clear an active HPV infection. Additionally, Category B encompasses patients experiencing systemic, chronic immunosuppression due to autoimmune conditions and subsequent therapeutic interventions. Individuals receiving long-term corticosteroid or biologic therapies for ailments such as systemic lupus erythematosus, rheumatoid arthritis, severe Crohn’s disease, or ulcerative colitis face a compromised cellular immune response, rendering them highly susceptible to HPV persistence and thus excellent candidates for routine cytological monitoring and subsequent HRA.
HRA for LGBTQ+ Patients
The intersection of specialized oncology and infectious disease disproportionately impacts the LGBTQ+ community, creating a profound necessity for highly accessible, culturally competent healthcare infrastructure. Within the specific domain of LGBTQ health Las Vegas, the proactive prevention of anal cancer represents one of the most pressing public health priorities.
Epidemiological research spanning multiple decades consistently and unequivocally identifies men who have sex with men (MSM) and transgender women as the demographic cohorts most uniquely vulnerable to the development of anal neoplasia. A comprehensive meta-analysis of contemporary clinical data reveals that the pooled incidence of anal cancer among MSM living with HIV is staggering, averaging 85.0 per 100,000 person-years. When the data is stratified by age, the risk amplifies dramatically; older MSM cohorts, specifically those aged 60 and above, face an incidence rate that frequently exceeds 107.5 per 100,000 person-years.
However, it is crucial to recognize that an HIV diagnosis is not the sole prerequisite for elevated risk. Among MSM who are entirely HIV-negative, the incidence of anal cancer remains substantially higher than that of the general heterosexual population. This elevated vulnerability is primarily attributed to the high transmission efficiency of the human papillomavirus during receptive anal intercourse, which introduces the pathogen directly into the delicate transition zone of the anal canal.
The baseline prevalence of highly oncogenic HPV strains within the asymptomatic LGBTQ+ population is a cause for intense clinical vigilance. Broad cohort studies indicate that among older MSM, nearly 47% exhibit underlying, unaddressed anal HSIL, and a full 19% are active carriers of the highly carcinogenic HPV-16 strain. These alarming epidemiological realities underscore the absolute necessity of integrating comprehensive anal dysplasia screening into routine, holistic sexual health maintenance. Patients actively engaging in other preventive health strategies, such as consulting a PrEP provider near you to access Pre-Exposure Prophylaxis for HIV prevention, or using Doxy-PEP (post-exposure doxycycline) to reduce bacterial STI risk, must concomitantly integrate HRA and HPV testing into their preventive care regimens.
Despite the glaring statistical need for these services, patients within the LGBTQ+ community frequently encounter formidable, systemic barriers when attempting to access adequate healthcare. These barriers encompass societal stigma, pervasive anxiety regarding invasive anogenital examinations, and a stark lack of general practitioners educated in the nuanced, highly specific health requirements of sexual minorities. A clinical environment dedicated to combating anal cancer must actively dismantle these barriers by providing care that is fundamentally affirming, deeply respectful, and entirely non-judgmental. By fostering a clinical atmosphere characterized by profound trust and absolute discretion, providers empower their patients to adhere strictly to the rigorous, long-term surveillance schedules required to effectively manage chronic HPV infections and definitively prevent malignant transformation.
HRA for People Living with HIV
The biological synergy that exists between the Human Immunodeficiency Virus and the Human Papillomavirus represents one of the most profound and complex clinical challenges in modern infectious disease management. Individuals living with HIV experience an extraordinarily compounded risk for developing anal neoplasia; clinical studies indicate that their baseline risk for developing anal cancer can be up to 37-fold higher than that of the uninfected general public. Mitigating this extraordinary risk is the central, driving focus for any dedicated HIV doctor Las Vegas who is committed to ensuring the long-term survivorship and quality of life of their patients.
To understand why this risk is so elevated, one must examine the precise immunological mechanisms at play. The human immune system relies heavily on a robust, coordinated cellular response—driven primarily by CD4+ T-lymphocytes—to identify, suppress, and ultimately clear transient HPV infections from the mucosal epithelium. HIV induces profound systemic immunosuppression by actively targeting, infecting, and depleting these exact CD4+ T-cells. In the presence of an active or historically unmanaged HIV infection, the body is structurally incapable of mounting the necessary immunological defense to eradicate the HPV virus. Consequently, the patient experiences persistent, chronic viral shedding and an accelerated, unhindered integration of the HPV DNA into the cellular genome of the anal mucosa.
Extensive longitudinal research illustrates that the depth and duration of this immune compromise are the primary drivers of cancer development. A longer overall duration of HIV infection, coupled with a history of a severely depleted nadir CD4 count, correlates directly and strongly with an exponentially increased risk of developing invasive anal cancer. Paradoxically, this oncological crisis is a byproduct of modern medical success. The widespread implementation and spectacular efficacy of modern highly active antiretroviral therapy (ART) have allowed people living with HIV to achieve near-normal life expectancies. Because these patients are no longer succumbing to acute AIDS-defining illnesses in their youth, they are now surviving long enough for the slow, decades-long pathophysiological progression of HPV-induced dysplasia to mature and manifest as invasive squamous cell carcinoma.
In direct response to this shifting epidemiological landscape and the definitive evidence provided by the ANCHOR trial, federal health authorities enacted a radical overhaul of national clinical standards. The U.S. Office of AIDS Research, operating in tandem with the CDC, implemented unprecedented updates to the official Opportunistic Infection guidelines. For the first time in medical history, explicit, highly structured anal cancer screening protocols were formally integrated into the fundamental baseline of routine HIV primary care.
These stringent federal guidelines mandate that all adults living with HIV must undergo an annual clinical assessment specifically designed to detect anal abnormalities, such as unexplained bleeding, chronic pain, or palpable masses, accompanied by a comprehensive Digital Anorectal Examination (DARE). Furthermore, for asymptomatic individuals who meet the established age thresholds (35 and older for MSM and transgender women; 45 and older for all other demographics), the protocol dictates mandatory laboratory-based screening. This typically involves an anal Pap smear or advanced high-risk HPV DNA co-testing, seamlessly integrated into their routine HIV care in Las Vegas. Should these preliminary laboratory evaluations reveal any presence of high-risk HPV or detect cellular atypia, the guidelines unequivocally require an immediate, prioritized referral for High-Resolution Anoscopy to perform visually targeted biopsies and facilitate precancer ablation.
What Happens During the Procedure?
For many patients, the anticipation of an anogenital diagnostic procedure generates significant psychological anxiety. A comprehensive, transparent understanding of the precise clinical steps involved in a High-Resolution Anoscopy can profoundly alleviate this apprehension while clearly demonstrating the diagnostic superiority of the intervention. The entire HRA examination is conducted seamlessly within an outpatient, in-office setting, and the core procedural elements typically require only 15 to 30 minutes to complete from start to finish.
Pre-Procedure Preparation
The accuracy and efficacy of an HRA rely heavily on optimal visualization of the anal mucosa. Therefore, meticulous pre-procedure preparation is vital. Beginning exactly seven days prior to the scheduled HRA, patients are strictly instructed to refrain from utilizing any anal interventions that could traumatize the tissue or obscure the cytology. This includes abstaining from the use of anal suppositories, internal enemas, medicated topical creams, and engaging in receptive anal intercourse.
Furthermore, patients must engage in a thorough medication review with their provider. Certain common pharmaceutical agents, specifically anticoagulants, NSAIDs like ibuprofen or high-dose aspirin, and high-dose supplements such as Vitamin E, possess blood-thinning properties that can significantly elevate the risk of prolonged bleeding if a biopsy becomes necessary. These medications may need to be temporarily paused under careful medical supervision. On the morning of the procedure, a normal, unforced bowel movement is highly recommended to naturally clear the lower rectum of fecal debris, though aggressive chemical bowel preps (like those required for colonoscopies) are entirely unnecessary.
Step-by-Step Clinical Workflow
- Patient Positioning and Initial Assessment: Upon entering the examination suite, the patient is asked to disrobe from the waist down and is provided with a modest clinical drape. The patient is then comfortably positioned on the examination table. The most universally utilized position for this procedure is the left lateral decubitus position, wherein the patient lies securely on their left side with their knees drawn firmly upward toward their chest, allowing for optimal anatomical exposure.
- Digital Anorectal Examination (DARE): The procedure commences with a thorough external visual inspection of the perianal skin to identify any obvious exophytic lesions, such as condyloma acuminata (warts). Following this, the clinician performs a Digital Anorectal Examination (DARE). Utilizing a highly lubricated, gloved finger, the clinician gently palpates the internal contours of the anal canal and lower rectum, feeling carefully for any sub-mucosal indurations, masses, or anatomical irregularities that cannot be visualized optically.
- Cytological Specimen Collection: If the patient has not undergone a recent anal Pap smear, the clinician will collect a cytological specimen. A sterile Dacron or polyester swab is gently inserted approximately two to three inches into the anal canal. The swab is rotated firmly against the mucosal walls to harvest superficial epithelial cells. This specimen is subsequently immersed in a liquid transport medium and dispatched to a laboratory to undergo both cytological grading and highly sensitive HPV DNA analysis.
- Application of Acetic Acid Contrast: Following cytology, the clinician inserts a small, well-lubricated tubular instrument called an anoscope into the anal canal. Once the anoscope is securely in place, the inner core (obturator) is withdrawn. A gauze pad or large cotton swab, heavily saturated with a 3% to 5% solution of acetic acid (a highly refined, medical-grade vinegar), is introduced through the anoscope and pressed firmly against the internal anal mucosa. The anoscope is then temporarily removed, leaving the acetic acid-soaked gauze in place for approximately one to two minutes. This step is chemically critical: acetic acid reacts aggressively with the high-density nuclear proteins that are the hallmark of dysplastic cells. Upon contact, these abnormal cells rapidly coagulate and turn stark white, a highly visible phenomenon clinically referred to as “acetowhitening”.
- Colposcopic Magnification and Lugol’s Iodine: The acetic acid gauze is carefully extracted, and the anoscope is reinserted. At this juncture, the colposcope is brought into position. The colposcope does not enter the body; rather, it remains externally positioned, projecting a brilliant beam of focused light through the hollow anoscope while providing dynamic optical magnification ranging from 10x to over 40x. Looking through the binocular optics or viewing the high-definition monitor, the clinician conducts an exhaustive millimeter-by-millimeter survey of the mucosa, mapping the acetowhite lesions and analyzing abnormal vascular capillary patterns.To further refine the tissue differentiation, a second chemical agent, Lugol’s iodine solution, may be applied. Healthy, mature squamous epithelial cells are rich in intracellular glycogen. When exposed to Lugol’s iodine, this glycogen absorbs the dye, causing the healthy tissue to stain a deep, dark mahogany brown. Conversely, dysplastic precancerous cells are rapidly dividing and completely glycogen-depleted; they reject the iodine stain and remain a pale, mustard yellow color, creating a stark visual boundary between healthy and diseased tissue.
- Targeted Biopsy and Hemostasis: Utilizing the high-resolution imagery and the vivid chemical contrast boundaries, the clinician isolates the specific areas of highest suspicion. A highly specialized, slender biopsy forceps is guided through the anoscope to precisely excise a microscopic tissue sample measuring only two to three millimeters in diameter. Because the biopsy creates a minute laceration in the highly vascular mucosal bed, immediate hemostasis is required. A localized chemical coagulant, most commonly Monsel’s solution (ferric subsulfate) or a silver nitrate applicator, is pressed directly onto the biopsy site to instantly halt localized capillary bleeding. The excised tissue sample is meticulously preserved in a formalin solution and dispatched to a specialized anatomical pathology laboratory for rigorous histological grading to definitively confirm the presence and severity of High-grade Squamous Intraepithelial Lesions (HSIL).
Is it Painful?
The paramount concern expressed by patients facing a High-Resolution Anoscopy is the acute anticipation of intense pain. However, a detailed understanding of lower gastrointestinal anatomy reveals why this procedure is, in fact, remarkably well-tolerated by the vast majority of patients. The perception of pain during an HRA is heavily dictated by a specific anatomical boundary known as the dentate line (or pectinate line).
The anal canal situated above the dentate line is lined with columnar and transitional epithelium and is innervated exclusively by the visceral nervous system. Crucially, visceral nerves lack the somatic sensory endings required to transmit sharp, acute pain signals. Consequently, clinical interventions, including firm pressure, the application of chemical acids, and even the mechanical excision of biopsy tissue in this upper region, generate sensations of dull pressure or mild, vague cramping rather than sharp pain.
Conversely, the tissue situated below the dentate line, extending outward to the perianal skin, is innervated by highly sensitive somatic nerves capable of registering acute pain. To entirely mitigate discomfort in this sensitive region, clinicians employ highly effective pharmacological strategies. Throughout the entirety of the examination, generous volumes of topical anesthetic gels, predominantly 2% or 5% lidocaine formulations, are applied liberally to numb the perianal epidermis and the lower anal canal. Due to the efficacy of these local anesthetics, systemic intravenous sedation or general anesthesia is virtually never required, allowing patients to remain fully conscious, communicative, and breathing independently throughout the procedure. If the clinician identifies a highly suspicious lesion located on the exterior perianal skin that requires biopsy, a tiny, localized subcutaneous injection of an anesthetic (such as lidocaine with epinephrine) will be administered with a micro-needle prior to tissue removal to ensure absolute comfort.
Post-Procedural Recovery and Aftercare
The recovery profile following a High-Resolution Anoscopy is exceptionally favorable. Because the procedure eschews general anesthesia, patients do not suffer from post-sedation grogginess and are invariably capable of driving themselves home and immediately resuming light, routine daily activities, including returning to professional office environments.
If a biopsy was excised during the examination, a specific set of minor, transient side effects is fully anticipated and easily managed:
- Minor Bleeding and Spotting: It is entirely normal to observe mild, bright red spotting on toilet tissue or minor streaking within the stool for the initial 24 to 48 hours. Furthermore, a secondary, highly localized slight bleed frequently occurs four to five days post-procedure as the internal chemical scab (formed by the Monsel’s solution) naturally sloughs off the healing mucosa.
- Localized Discomfort: A sensation of dull, deep aching, mild throbbing, or localized soreness within the anal canal may persist for several days. This discomfort rarely requires prescription analgesics and is highly responsive to standard over-the-counter pain relievers such as acetaminophen.
- Activity Restrictions: To facilitate optimal mucosal healing and prevent the mechanical tearing of the fragile biopsy sites, patients are strictly advised to abstain from any strenuous physical exertion, including heavy lifting (objects exceeding 20 pounds), high-impact cardiovascular exercise, and swimming in public pools for a minimum of one week. Most importantly, patients must absolutely abstain from receptive anal intercourse and the insertion of any anal toys, fingers, or non-prescribed suppositories during this healing window.
- Dietary and Hygiene Adjustments: Maintaining soft, easily passable stools is the most critical factor in a comfortable recovery. Patients are strongly encouraged to temporarily increase their intake of dietary fiber, maintain robust daily hydration, and proactively utilize over-the-counter osmotic stool softeners to completely eliminate the need for straining during defecation. To alleviate localized soreness and promote circulation, patients may take frequent sitz baths—sitting in a few inches of plain, warm water—multiple times a day as needed.
Cost & Insurance in Las Vegas
Navigating the financial and logistical complexities of specialized healthcare is a critical, and often stressful, step for patients seeking preventive interventions. The total comprehensive cost of a High-Resolution Anoscopy is highly variable and is influenced by the clinical complexity of the individual procedure, the necessity for single or multiple pathological biopsies, the utilization of laser ablation therapies, and the specific parameters of the patient’s insurance coverage network.
Clinical Coding and Documentation
Insurance reimbursement, pre-authorization, and standardized medical billing for HRA are strictly governed by specific Current Procedural Terminology (CPT) codes, which are established and maintained by the American Medical Association. Accurate, meticulous clinical coding ensures that the precise medical necessity of the complex procedure is transparently communicated to the health insurance payer.
The primary CPT codes associated with this procedure include:
- CPT Code 46601: Diagnostic anoscopy with high-resolution magnification (HRA) and chemical agent enhancement, including the collection of superficial specimens by brushing or washing, but entirely excluding the excision of a tissue biopsy.
- CPT Code 46607: Anoscopy with high-resolution magnification (HRA) and chemical agent enhancement, explicitly including the excision of single or multiple targeted biopsies.
- CPT Code 46924: The extensive surgical destruction of anal lesions (including condyloma or severe dysplasia) utilizing advanced methodologies such as laser surgery, electrosurgery, or cryosurgery.
| Procedure Code | Clinical Description | Typical Global Surgical Period |
| CPT 46601 | Diagnostic HRA without biopsy | 0-day |
| CPT 46607 | HRA including single/multiple biopsies | 0-day |
| CPT 46924 | Extensive destruction/ablation of anal lesions | 10-day |
Standard procedural coding metrics utilized for insurance authorization and revenue cycle management.
Federal Medicare Administrative Contractors and the vast majority of private, commercial health insurers universally provide coverage for CPT codes 46601 and 46607, provided that highly specific, stringent medical necessity criteria are meticulously documented in the patient’s chart. These rigorous criteria typically mandate a documented clinical history of HPV-related anal disease (such as prior surgeries for anal warts), the presence of verifiable abnormalities on a recent anal Pap smear (cytology), or the discovery of palpable irregularities detected by a physician during a Digital Anorectal Examination. It is crucial to note that insurers almost universally classify HRA as an experimental or investigational intervention if it is utilized purely as an initial, asymptomatic screening tool in low-risk populations; therefore, a standard, low-cost cytological swab must consistently precede the HRA in routine diagnostic workflows to secure insurance authorization.
Insurance Networks in Nevada
Patients residing within the expansive Las Vegas metropolitan area benefit from access to a highly diverse array of commercial, state-sponsored, and federal insurance plans that facilitate robust coverage for advanced specialist procedures. Recognizing the local insurance landscape empowers patients to coordinate their specialized care efficiently and avoid unexpected financial burdens.
- Nevada Medicaid: Managed Care Organizations (MCOs) operating under the umbrella of Nevada Medicaid—most notably Anthem Blue Cross and Blue Shield and the Health Plan of Nevada (HPN)—provide comprehensive coverage for essential diagnostic services, which explicitly includes outpatient specialist procedures like HRA.
- Commercial and Marketplace Plans: The state-run Nevada Health Link offers a wide variety of ACA-compliant plans that robustly cover essential preventive screenings and necessary diagnostic follow-ups. Major commercial carriers operating in the region include SilverSummit Healthplan, Hometown Health, SelectHealth, and Imperial Health Plan.
- Medicare Advantage: For older populations transitioning into retirement, specialized Medicare Advantage plans operated by Optum Nevada, Humana, and AARP/UnitedHealthcare offer highly integrated, comprehensive coverage networks that encompass highly specialized infectious disease and proctology providers who routinely perform HRA.
Patients are strongly advised to proactively contact their insurance provider to verify that their specific health plan covers out-patient diagnostic endoscopies, to comprehend their specific deductible and co-insurance obligations, and to firmly confirm any required prior authorizations with their referring primary care physician or via a preliminary consultation prior to the procedure.
Considerations for Self-Pay Patients
For uninsured patients, or those burdened by exceptionally high-deductible health plans, navigating direct out-of-pocket costs is a vital necessity. Healthcare transparency marketplaces and self-pay pricing models published by major urgent care networks in Las Vegas indicate that complex, high-tier diagnostic visits typically range from $230 to $350 simply for the clinical encounter and basic in-house diagnostics. However, it is critical to understand that highly specialized, sub-specialty procedures like High-Resolution Anoscopy are generally billed at significantly higher specialist rates due to the extensive training required and the immense cost of the sophisticated optical equipment utilized. Furthermore, these base procedural estimates rarely include the substantial external laboratory fees required for the intricate pathological evaluation of the excised biopsies. Patients paying entirely out-of-pocket should consult directly and transparently with the facility’s billing department prior to their appointment to inquire about tiered pricing structures, self-pay discounts, or bundled service rates that comprehensively encompass both the HRA procedure and the subsequent pathology components.
Why Choose Farabi Wellness Center?
When a patient is required to select a healthcare provider for an incredibly intricate, highly technical procedure such as High-Resolution Anoscopy, the intersection of specialized clinical expertise and cutting-edge technological capability is absolutely paramount. Farabi Wellness Center has meticulously established itself as a distinguished, highly specialized clinical hub dedicated to advanced infectious disease management and proactive anal neoplasia prevention within Southern Nevada.
Unparalleled Clinical Expertise
The operational and clinical foundation of the center’s excellence is its founder and primary physician, Dr. Alireza Farabi. Operating as a board-certified, actively practicing Infectious Disease specialist with a career spanning over 25 years of rigorous medical experience, Dr. Farabi possesses an extraordinarily nuanced, systemic understanding of complex virology, human immunology, and the devastating, highly intricate interplay between HIV and HPV. This deep, systemic comprehension ensures that patients receive holistic, comprehensive care that aggressively addresses both the immediate, visible dysplastic lesions and the underlying, invisible immunological deficiencies driving the progression of the disease.
Furthermore, Farabi Wellness Center proudly highlights its strategic clinical affiliations with elite, globally recognized academic researchers, including Dr. J. Michael Berry-Lawhorn. As a Clinical Professor of Medicine at the University of California, San Francisco (UCSF) and a globally recognized, pioneering authority in hematology, oncology, and anal neoplasia research, Dr. Berry-Lawhorn’s affiliation elevates the clinical standard of the facility. Access to such high-caliber, bleeding-edge academic insight ensures that the clinic operates strictly according to the latest, most advanced medical paradigms and treatment algorithms available globally.
Advanced Technological Infrastructure
The diagnostic precision and ultimate clinical success of a High-Resolution Anoscopy rely almost entirely upon the optical quality and mechanical refinement of the instruments utilized by the physician. Recognizing this technological imperative, Farabi Wellness Center has heavily invested in the THD ProctoStation and THD HRStation, which are universally regarded as state-of-the-art, deeply integrated proctological platforms designed specifically for the rigorous screening and laser treatment of anal precancerous lesions.
The deployment of the THD HRStation provides the clinic with remarkable, undeniable technological advantages:
- 4K Ultra-High Definition Video Resolution: The system features a high-performance, integrated workstation equipped with an advanced 4K video camera. This optical powerhouse provides uncompromised, hyper-detailed visualization of the anal mucosa, displaying the microscopic vascular architecture on a massive 32-inch UHD 4K monitor, completely eliminating visual ambiguity for the operating physician.
- Integrated LED Cold Light Technology: The system utilizes the disposable THD Light-Scope Procto HRA, a revolutionary proctoscope that entirely eliminates the need for cumbersome external light cables. Its powerful, built-in LED source delivers intense, highly focused illumination directly to the target tissue without emitting any thermal heat, drastically maximizing patient safety and ensuring absolute comfort during prolonged examinations.
- Atraumatic, Single-Use Design: The single-use, instantly ready-to-use proctoscope features a highly refined atraumatic profile, ensuring a smooth, vastly more comfortable insertion for the patient while entirely eliminating the logistical nightmares and severe risks associated with equipment cross-contamination and inadequate sterilization.
- Seamless Laser Ablation Compatibility: The diagnostic system seamlessly integrates with the formidable THD Laser Station. This allows the physician to transition instantly from diagnosis to treatment, utilizing a highly precise CO2 laser emitting a 10.6-micrometer wavelength to instantly ablate high-grade anal intraepithelial lesions the moment they are definitively identified, ensuring rapid, highly effective treatment in a single clinical setting.
| THD ProctoStation Technical Specifications | System Capabilities |
| Operating System & Storage | Windows 10 Pro, 1TB Hard Disk, 8GB RAM |
| Magnification Power | 13.8X up to 40X Optical Zoom |
| Illumination Source | Integrated LED Cold-Light (No external thermal output) |
| Ablation Integration | CO2 Laser Station (10.6 micrometers wavelength) |
A Fiercely Patient-Centric Clinical Model
Beyond the impressive technological acquisitions and academic expertise, the daily operational philosophy of the clinic is meticulously engineered to cater specifically to patient convenience, profound privacy, and total psychological safety. Recognizing the terrifying urgency often associated with abnormal diagnostic findings, the clinic administration strives tirelessly to offer same-week appointments, drastically reducing the agonizing waiting periods that typically exacerbate severe patient anxiety.
The entire clinical team operates with a fierce, unwavering commitment to non-judgmental, fully inclusive medicine. Serving as a prominent, trusted fixture in LGBTQ health Las Vegas, the staff ensures an environment where complex sexual health histories, intimate behaviors, and infectious disease statuses are discussed openly, highly respectfully, and with absolute confidentiality. Whether a patient requires a routine screening,, specialized lifelong HIV management, or an urgent, highly time-sensitive PEP (Post-Exposure Prophylaxis) consultation, the care is delivered with uncompromising compassion and absolute medical precision.
When to Schedule Screening
In the realm of oncology and preventive infectious disease, clinical timing is the absolute determining factor between a minor outpatient intervention and a life-altering cancer diagnosis. For patients who fit into the established high-risk epidemiological categories, perpetually deferring screening allows microscopic, highly treatable cellular dysplasia to silently mature into aggressive, life-threatening malignancies.
- Individuals Living with HIV: A comprehensive baseline assessment, encompassing a detailed symptom review and a DARE, must be performed annually. Laboratory screening (anal cytology) must commence rigorously at age 35 for MSM and transgender women, and at age 45 for all other individuals living with HIV.
- Immunocompromised Individuals: Solid organ transplant recipients, as well as those reliant on heavy, systemic immunosuppressants for autoimmune disorders, should initiate urgent, proactive conversations regarding regular screening protocols with their primary specialist immediately upon assuming their medication regimen.
- History of HPV-Related Disease: Individuals of any gender with a documented historical diagnosis of anogenital warts or cervical/vulvar dysplasia should proactively demand an evaluation from their provider.
If a routine cytology swab returns a positive laboratory result for highly oncogenic high-risk HPV, or indicates any degree of cellular atypia (such as ASC-US, LSIL, or HSIL), a High-Resolution Anoscopy must be scheduled promptly to visually confirm the pathology and biopsy the affected mucosal tissue.
If you’re unsure of your status, start with HIV Testing and Diagnosis before advanced screening.
FAQs
To further clarify the highly technical clinical nuances of High-Resolution Anoscopy Las Vegas, the following frequently asked questions provide concise, medically accurate answers regarding the complex procedure and its widespread public health applications.
What is the definitive difference between standard anoscopy and High-Resolution Anoscopy?
Standard anoscopy utilizes a simple, hollow plastic tube and a basic external flashlight to visually inspect the anal canal for large, macroscopic structural issues like bleeding hemorrhoids or deep fissures. High-Resolution Anoscopy (HRA) is vastly more complex; it pairs the anoscope with a high-powered, binocular magnifying colposcope and specific chemical contrast agents (acetic acid and Lugol’s iodine) to illuminate and detect microscopic, precancerous cellular mutations caused by HPV. HRA is the only recognized method for visually identifying early anal dysplasia.
Exactly how long does a comprehensive HRA procedure take?
The HRA procedure is conducted entirely within an outpatient, private office setting and typically requires a brief 15 to 30 minutes to complete from the initial examination to the final biopsy hemostasis. The overall duration may extend slightly by a few minutes if the physician identifies widespread multifocal disease and determines that multiple, distinct biopsies are medically necessary to properly evaluate the suspicious lesions.
Can I immediately return to my job after an HRA in Las Vegas?
Yes. Because the procedure exclusively utilizes highly localized topical anesthetics (such as 5% lidocaine gel) and does not require any form of general sedation or intravenous anesthesia, patients remain fully alert and maintain total physical autonomy. The vast majority of individuals comfortably resume normal daily activities, including returning to professional environments and operating motor vehicles, immediately following the conclusion of the appointment.
Does my health insurance plan cover High-Resolution Anoscopy?
Yes, when strict, documented medical necessity criteria are met. Medicare, state-run Medicaid programs (including Nevada MCOs like SilverSummit and Anthem), and major commercial insurers typically authorize and cover diagnostic HRA (CPT 46601) and HRA with targeted biopsy (CPT 46607) if the patient presents with abnormal anal cytology results, palpable anatomical abnormalities discovered during a rectal exam, or a heavily documented medical history of severe HPV-related disease.
How frequently should anal dysplasia screening be performed by a specialist?
The frequency of screening depends entirely on the patient’s individual immunological risk profile and the specific results of prior pathology reports. High-risk individuals, such as MSM living with HIV over the age of 35, are strictly advised to undergo an annual Digital Anorectal Exam and concurrent cytology screening. If a subsequent HRA yields entirely normal findings, the patient may safely return to standard annual cytological surveillance; conversely, abnormal histological findings will dictate a highly customized, accelerated follow-up timeline determined directly by the treating physician.
Is an aggressive chemical bowel preparation required before an HRA?
Rigorous, highly uncomfortable bowel preparation, such as the intense, high-volume liquid laxative regimens mandated prior to colonoscopies, is completely unnecessary for an HRA. Patients are simply advised to have a normal, unforced bowel movement on the morning of their procedure. To ensure optimal mucosal visibility and accuracy, patients must strictly avoid using internal enemas, medicated anal creams, or engaging in receptive anal intercourse for seven full days prior to the examination.
Conclusion
The relentlessly rising incidence of HPV-related anal neoplasia across the United States demands a highly sophisticated, aggressively proactive approach to public healthcare. High-Resolution Anoscopy represents the absolute pinnacle of diagnostic precision within this field, enabling highly trained clinicians to intercept, map, and eradicate precancerous cellular lesions long before they possess the capability to progress into invasive, life-threatening malignancies. The definitive, unimpeachable data provided by the landmark ANCHOR study has irrevocably proven that the active clinical identification and immediate treatment of anal HSIL is a profoundly life-saving protocol, particularly for highly vulnerable, heavily burdened populations such as MSM, transgender women, and individuals living with HIV.
Within the Las Vegas metropolitan area, reliable access to this highly specialized, life-saving procedure is streamlined through dedicated, technologically advanced facilities. Through a rare combination of profound clinical infectious disease expertise, advanced 4K optical colposcopic technology, and an unwavering, deeply entrenched commitment to compassionate, affirming patient care, the optimal environment for complex oncological prevention is firmly established.
Do not defer critical, potentially life-saving preventive care due to anxiety or a lack of specialized information. Early clinical detection through precision optical technology guarantees the highest possible probability of maintaining long-term health, surviving high-risk viral infections, and ensuring total peace of mind.
Schedule your High-Resolution Anoscopy consultation in Las Vegas today with Dr. Alireza Farabi at Farabi Wellness Center.